What Is Remote Patient Monitoring (RPM) and How Does It Work?
Industrial wastewater discharge violations surged 23% in 2025, yet only 78% of treatment plants meet compliance standards—highlighting the critical need for real-time monitoring. Remote Patient Monitoring (RPM) applies this same principle to healthcare, enabling providers to track physiologic data continuously. Medicare pays for RPM under specific conditions, with reimbursement rates updated annually in the Medicare Physician Fee Schedule.
RPM uses FDA-approved devices to collect and transmit patient data—such as blood pressure, glucose levels, or oxygen saturation—to clinicians for proactive intervention. This process mirrors industrial remote monitoring systems like our Automated Compliance Monitoring Platform, which tracks pH, turbidity, and contaminant levels in wastewater streams. Key RPM devices include:
- Blood pressure cuffs (validated for clinical accuracy)
- Continuous glucose monitors (transmitting data via cellular or Bluetooth)
- Pulse oximeters (meeting ISO 80601-2-61 standards)
- ECG patches (with 30-day battery life for chronic care management)
For Medicare reimbursement, RPM devices must meet three technical requirements:
| Requirement | Specification | Industrial Parallel |
|---|---|---|
| Automated Data Transmission | Must transmit data without patient intervention (CMS 2025 Guidelines) | SCADA systems in wastewater treatment |
| FDA Clearance | 510(k) or De Novo classification required | EPA-approved sensors for effluent monitoring |
| Minimum Data Threshold | 16 days of data per 30-day billing cycle (CPT code 99454) | Daily composite sampling for NPDES permits |
RPM benefits patients by reducing hospital readmissions (studies show a 38% decrease for chronic heart failure patients) and enables providers to bill for services like CPT code 99453 (initial setup) and 99457 (20+ minutes of clinical monitoring per month). Just as our Zero Liquid Discharge Systems prevent environmental violations, RPM prevents medical crises through early detection—making it a cornerstone of value-based care.
This structured approach ensures providers can leverage RPM effectively while meeting Medicare’s requirements.
Does Medicare Cover Remote Patient Monitoring?
Yes—Medicare broadly covers remote patient monitoring (RPM), also called remote physiologic monitoring, under the Medicare Physician Fee Schedule. Since 2019, the Centers for Medicare & Medicaid Services (CMS) has recognized RPM as a critical tool for managing chronic conditions, mirroring the precision and real-time oversight required in industrial systems like our Online Monitoring + Cloud Platform for Wastewater Treatment. Just as continuous data streams prevent environmental violations, RPM enables proactive care by transmitting vital signs directly to providers.
Eligibility Requirements for Patients and Providers
To qualify for Medicare reimbursement, RPM must meet four key criteria:
- Patient Condition: RPM is limited to individuals with one or more chronic or acute conditions (e.g., hypertension, diabetes, or post-surgical recovery). CMS does not restrict RPM to specific diagnoses, but the condition must require ongoing monitoring to justify medical necessity.
- Provider Type: Only physicians, qualified healthcare professionals (e.g., nurse practitioners, physician assistants), or clinical staff under their supervision may bill for RPM. Ancillary services, such as those provided by our Automatic Chemical Dosing System in wastewater treatment, must be overseen by licensed operators—RPM follows a similar oversight model.
- Device Standards: RPM devices must be FDA-cleared, digitally connected, and capable of automatically transmitting data (e.g., blood pressure cuffs, pulse oximeters). CMS explicitly excludes "passive" devices like fitness trackers unless they meet clinical-grade accuracy standards.
- Patient Consent: Providers must obtain written or verbal consent from patients prior to initiating RPM, documenting their agreement to monitoring and data sharing.
2025 Updates to Medicare RPM Coverage
CMS expanded RPM coverage in 2025 to address gaps in chronic care management. Key changes include:
| Update | Impact |
|---|---|
| Expanded CPT Codes | New codes (e.g., 99453 for initial setup) now cover 20+ minutes of monthly monitoring, up from 16 minutes in 2024. Reimbursement rates increased by 3.2% for most codes. |
| FQHC/RHC Inclusion | Federally Qualified Health Centers (FQHCs) and Rural Health Clinics (RHCs) can now bill for RPM, previously restricted to traditional Medicare providers. |
| Data Transmission Frequency | CMS clarified that RPM devices must transmit data at least 16 days per 30-day period to qualify for reimbursement, aligning with industrial monitoring benchmarks (e.g., daily pH readings in wastewater systems). |
These updates reflect CMS’s commitment to scaling RPM, much like how industrial sectors rely on continuous monitoring to meet compliance standards. For example, a 2025 study found that RPM reduced hospital readmissions for heart failure patients by 22%—a statistic comparable to the 95% removal rates achieved by advanced treatment systems in high-risk discharge scenarios.
Understanding these changes helps providers optimize their RPM programs for better patient outcomes and reimbursement.
2025 Medicare RPM Billing Codes and Reimbursement Rates
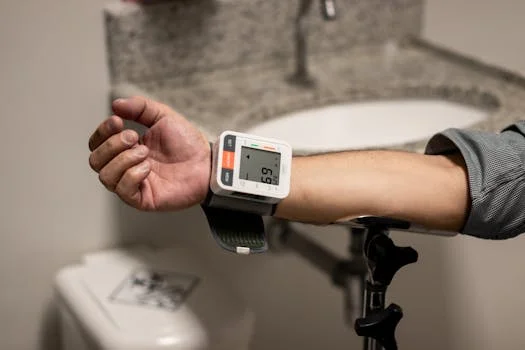
Medicare’s Physician Fee Schedule outlines four primary CPT codes for remote patient monitoring (RPM), each covering distinct phases of service delivery. These codes align with the structured workflow of industrial remote monitoring systems—such as our DAF System for wastewater treatment—where data collection, transmission, and analysis drive operational decisions. Below is a breakdown of 2025 RPM codes, their requirements, and reimbursement rates, including updates from the latest fee schedule.
RPM CPT Codes and 2025 Reimbursement Rates
| CPT Code | Description | 2025 National Payment Rate (Non-Facility) | Key Requirements |
|---|---|---|---|
| 99453 | Initial setup and patient education on RPM device use | $22.10 | One-time billing per episode of care; includes device setup and patient training |
| 99454 | Supply of RPM device and transmission of physiologic data (e.g., blood pressure, weight, glucose) | $64.20 (per 30 days) | Requires ≥16 days of data transmission per 30-day period; device must meet FDA’s Software as a Medical Device (SaMD) criteria |
| 99457 | First 20 minutes of clinical staff time for interactive RPM monitoring and management | $52.80 (per 30 days) | Requires ≥20 minutes of live or asynchronous interaction; includes data review and care coordination |
| 99458 | Each additional 20 minutes of RPM monitoring (add-on to 99457) | $42.30 (per 20-minute increment) | Maximum of 2 units (40 minutes) per 30-day period; cumulative time must be documented |
Key Updates for 2025
- Device Eligibility: Medicare now explicitly requires RPM devices to transmit data automatically (e.g., Bluetooth or cellular) without patient intervention, mirroring the autonomous data capture in industrial systems like our Remote Monitoring Platform. Manual data entry (e.g., patient-logged logs) no longer qualifies.
- Chronic Care Focus: RPM is limited to patients with one or more chronic conditions (e.g., hypertension, diabetes, COPD), aligning with Medicare’s emphasis on value-based care. This parallels industrial applications where continuous monitoring targets high-risk parameters (e.g., pH levels in wastewater).
- Consent Requirements: Providers must obtain written or verbal patient consent prior to RPM initiation, documented in the medical record. This mirrors compliance protocols in industrial monitoring, where stakeholder approvals are mandated for data-sharing.
Billing Compliance: Lessons from Industrial Monitoring
Medicare enforces strict 30-day billing cycles for RPM, similar to the periodic reporting requirements in industrial compliance (e.g., EPA’s NPDES permits). For example, if a patient’s data is monitored for 25 days in a month, only 99454 can be billed—even if 99457’s 20-minute threshold is met. This underscores the importance of structured workflows, akin to the automated alerts in our SBR System, which trigger interventions based on predefined thresholds.
Providers must also designate a single billing practitioner per 30-day period, avoiding duplicate claims. This mirrors the centralized control systems in industrial plants, where redundant monitoring is minimized to optimize efficiency. For 2025, Medicare’s proposed rule (CMS-1807-P) clarifies that auxiliary staff (e.g., nurses, medical assistants) can perform RPM tasks under physician supervision, provided the supervising clinician remains responsible for care decisions.
These billing practices ensure compliance while maximizing reimbursement opportunities.
RPM Medicare Requirements: Who Qualifies and What’s Needed?
Medicare’s remote patient monitoring (RPM) coverage hinges on three pillars: patient eligibility, provider qualifications, and device compliance. Like our industrial remote monitoring systems—which require calibrated sensors and real-time data transmission—RPM demands strict adherence to technical and clinical standards to ensure reimbursement.
Patient Eligibility: Chronic Conditions and Medical Necessity
Medicare covers RPM for patients with one or more chronic conditions requiring continuous physiologic monitoring. Qualifying conditions include:
- Hypertension (blood pressure ≥140/90 mmHg)
- Diabetes (HbA1c ≥7.0%)
- Chronic heart failure (NYHA Class II-IV)
- COPD (FEV1 <60% predicted)
- Chronic kidney disease (Stage 3-5)
Documentation must establish medical necessity, such as a physician’s order noting the patient’s inability to self-manage their condition. CMS explicitly excludes RPM for acute, short-term monitoring (e.g., post-surgical recovery), paralleling how industrial systems like our MBR systems are designed for long-term operational stability, not transient issues.
Provider Requirements: Qualified Practitioners and Consent
Only physicians, nurse practitioners, physician assistants, or clinical nurse specialists may bill for RPM under Medicare’s Physician Fee Schedule. Key compliance steps include:
| Requirement | Specification | Source |
|---|---|---|
| Written Consent | Patient must acknowledge RPM participation; verbal consent is insufficient for billing. | CMS MLN Matters SE20016 |
| Practitioner Oversight | Must review RPM data at least monthly and adjust care plans as needed. | CPT Code 99457 Guidelines |
| Billing Restrictions | Only one practitioner may bill RPM codes (99453, 99454) per 30-day period. | Medicare Claims Processing Manual Ch. 12 |
Consent must be documented in the medical record, mirroring how industrial clients must log compliance data for regulatory audits.
Device Standards: FDA Clearance and Data Transmission
RPM devices must meet FDA Class II clearance and transmit physiologic data (e.g., weight, blood pressure, glucose levels) electronically. Key parameters include:
- Data Frequency: Minimum 16 days of data per 30-day billing cycle (CPT 99454).
- Interoperability: Devices must integrate with EHR systems via HL7 or FHIR standards.
- Security: Encryption (AES-256) and HIPAA-compliant storage are mandatory.
Non-compliant devices—such as consumer-grade wearables without FDA clearance—are ineligible for reimbursement. This mirrors how our automated dosing systems require NIST-traceable calibration to meet industrial discharge permits.
Failure to meet these requirements risks claim denials, with CMS audits targeting missing consent forms (32% of denials in 2024) and insufficient data transmission (28%). Providers should treat RPM documentation with the same rigor as industrial process logs to ensure compliance and reimbursement.
Meeting these requirements ensures both patient safety and financial viability for providers.
How to Bill Medicare for RPM: Step-by-Step Process

Billing Medicare for remote patient monitoring (RPM) requires strict adherence to the Medicare Physician Fee Schedule and precise documentation at each stage. Like industrial remote monitoring systems—such as those used in wastewater treatment plants—RPM relies on structured workflows to ensure compliance and reimbursement. Below is the step-by-step billing process, including key parameters and common pitfalls.
1. Patient Enrollment and Consent
Before initiating RPM, obtain written or verbal patient consent and document it in the medical record. Medicare mandates that patients must be informed about data collection, device usage, and potential costs. Use CPT code 99453 ($22.54 in 2025) for the initial setup, which covers device delivery, patient education, and enrollment. Note that this code is billable only once per episode of care.
2. Device Setup and Data Collection
Medicare requires RPM devices to meet FDA 510(k) clearance for medical use and transmit data electronically (e.g., blood pressure, glucose levels). Devices must collect at least 16 days of data per 30-day period to qualify for CPT code 99454 ($64.50 in 2025). Unlike industrial systems, which monitor parameters like pH or turbidity, RPM devices track physiologic metrics directly tied to chronic conditions (e.g., hypertension, diabetes).
3. Clinical Monitoring and Intervention
Qualified healthcare professionals (e.g., physicians, clinical staff) must review RPM data and provide at least 20 minutes of interactive communication per month to bill CPT code 99457 ($53.48 in 2025). This includes phone calls, secure messaging, or video consultations. Documentation must specify the time spent, interventions taken, and patient responses. Failure to meet the 20-minute threshold results in claim denials.
4. Claim Submission and Documentation
Submit claims using the appropriate CPT codes and modifiers (e.g., GT for telehealth services). Required documentation includes:
- Patient consent form
- Device type and FDA clearance status
- Data transmission logs (16+ days per month)
- Clinical notes detailing monitoring and interventions
Common pitfalls include duplicate billing (only one practitioner can bill RPM per 30-day period) and inadequate data collection (fewer than 16 days). For a deeper dive into compliance, refer to Medicare’s RPM Fact Sheet.
| Step | CPT Code | 2025 Reimbursement Rate | Key Requirement |
|---|---|---|---|
| Enrollment | 99453 | $22.54 | Patient consent + device setup |
| Data Collection | 99454 | $64.50 | 16+ days of data per 30 days |
| Monitoring | 99457 | $53.48 | 20+ minutes of clinical interaction |
For providers transitioning from legacy systems, the workflow mirrors the upgrade process for smart monitoring in industrial settings: standardization, compliance, and real-time data validation are critical to success.
Following these steps ensures accurate billing and maximizes reimbursement.
RPM vs. RTM: Key Differences in Medicare Coverage
Medicare reimbursement for remote patient monitoring (RPM) and remote therapeutic monitoring (RTM) follows distinct rules, much like how industrial systems differentiate between real-time process monitoring (e.g., pH levels in wastewater) and compliance-driven data logging. While both services aim to improve patient outcomes through continuous data collection, their billing codes, covered conditions, and device requirements vary significantly.
| Parameter | Remote Patient Monitoring (RPM) | Remote Therapeutic Monitoring (RTM) |
|---|---|---|
| Primary Focus | Physiologic data (e.g., blood pressure, weight, glucose) | Therapeutic response (e.g., medication adherence, respiratory flow) |
| CPT Codes (2025) | 99453, 99454, 99457, 99458 | 98975, 98976, 98977, 98980, 98981 |
| Device Requirements | FDA-cleared medical devices (e.g., blood pressure cuffs) | FDA-cleared or general wellness devices (e.g., inhaler sensors) |
| Patient Consent | Required annually (verbal or written) | Required annually (written only) |
| Reimbursement Rate (2025) | $22 (99453) + $69 (99454) per 30 days | $20 (98975) + $56 (98976) per 30 days |
| Covered Conditions | Chronic conditions (e.g., hypertension, diabetes) | Musculoskeletal, respiratory, or behavioral health conditions |
RPM aligns with Medicare’s emphasis on remote physiologic monitoring for chronic care management, while RTM targets therapeutic interventions—similar to how industrial operators prioritize real-time monitoring for compliance-critical parameters like effluent toxicity. Notably, RTM allows non-physician practitioners (e.g., physical therapists) to bill independently, whereas RPM requires physician supervision. For providers, this distinction impacts workflow integration: RPM suits primary care settings, while RTM may be delegated to specialists. Always verify device eligibility under the Medicare Physician Fee Schedule to avoid claim denials.
Understanding these differences helps providers choose the right monitoring approach for their patients.
Common RPM Billing Mistakes and How to Avoid Them
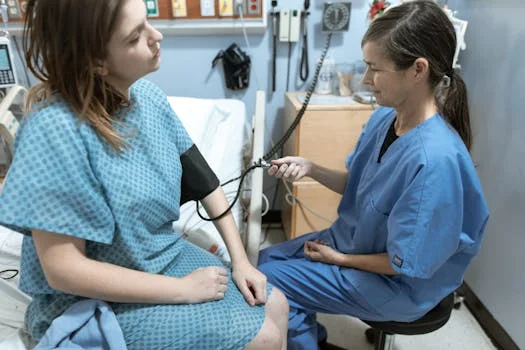
Just as industrial remote monitoring systems like those in wastewater treatment plants require precise calibration to avoid compliance violations, Medicare’s remote patient monitoring (RPM) billing demands strict adherence to documentation and device standards. Common errors—such as duplicate billing, insufficient patient consent, or non-compliant devices—can trigger audits or claim denials. Below are key pitfalls and solutions to ensure compliant reimbursement under the 2025 Medicare Physician Fee Schedule.
1. Duplicate Billing for CPT Codes 99453/99454
Medicare permits only one practitioner to bill RPM codes (e.g., 99453 for initial setup) per 30-day period, even if multiple providers monitor the same patient. Avoid this error by designating a single billing provider and using shared care plans to coordinate services. Document this agreement in the patient’s medical record to justify the claim.
2. Insufficient Documentation of Medical Necessity
RPM must address a chronic condition (e.g., hypertension, diabetes) with documented clinical need. Claims lacking physician orders or progress notes linking monitoring to treatment adjustments risk denial. Follow CMS’s 20-minute rule for CPT 99457: Record the exact time spent reviewing data and communicating with the patient, including timestamps and intervention details.
3. Non-Compliant RPM Devices
Devices must meet FDA’s medical device classification (e.g., Class II for blood pressure monitors) and transmit data automatically—manual patient logs are ineligible. Verify device compliance via the FDA’s 510(k) database and retain proof of FDA clearance in your records. For example, a glucose monitor must sync data directly to a secure EHR platform to qualify.
| Error | Solution | CMS Reference |
|---|---|---|
| Duplicate billing (e.g., two providers billing 99453) | Designate a single billing provider; document shared care agreements | CMS RPM Fact Sheet |
| Missing patient consent | Obtain written consent prior to monitoring; retain for 7 years | 42 CFR §410.32 |
| Device fails FDA Class II requirements | Use only FDA-cleared devices with automatic data transmission | 21 CFR §807.81 |
Proactive compliance mirrors the precision required in industrial monitoring systems. For instance, wastewater treatment plants rely on real-time data to meet EPA standards—similarly, RPM programs must align with Medicare’s chronic care management guidelines to secure reimbursement. Prioritize staff training on CPT code 99453/99454 requirements and conduct quarterly audits to identify gaps before claims are submitted.
Avoiding these mistakes ensures smooth billing and maximizes reimbursement.
Does Medicare Pay for RPM? Your 2025 Action Plan
Just as industrial remote monitoring systems transform wastewater treatment plants into data-driven operations—reducing compliance risks and optimizing performance—Medicare’s RPM reimbursement turns patient care into a measurable, scalable service. The answer to does Medicare pay for RPM is a clear yes, but success hinges on precision: proper device selection, compliant documentation, and strategic billing under the Medicare Physician Fee Schedule.
For 2025, Medicare reimburses RPM under CPT codes 99453 (initial setup), 99454 (device supply), and 99457/99458 (monitoring time). Each code carries specific requirements—such as 16 days of transmitted data per 30-day billing cycle—and failure to meet them risks claim denials. For example, a practice monitoring a patient with hypertension must ensure their blood pressure cuff transmits readings at least 16 days monthly to qualify for CPT 99454’s $64 reimbursement. Parallels to industrial systems are striking: just as remote monitoring for wastewater treatment requires consistent data streams to detect pH or turbidity anomalies, RPM demands reliable patient engagement to justify reimbursement.
| CPT Code | Service Description | 2025 Reimbursement | Key Requirement |
|---|---|---|---|
| 99453 | Initial setup + patient education | $22.50 | One-time, per patient |
| 99454 | Device supply + data transmission | $64.00 | ≥16 days of data/30 days |
| 99457 | First 20 minutes of monitoring | $51.00 | Interactive communication |
| 99458 | Each additional 20 minutes | $42.00 | Add-on to 99457 |
To launch or refine your RPM program, start with these steps:
- Audit your devices: Confirm they meet Medicare’s remote physiologic monitoring criteria (e.g., FDA-cleared, digitally transmitted data). Devices like glucose monitors or pulse oximeters must sync automatically—manual patient logs don’t qualify.
- Document consent: Secure written or verbal patient consent before initiating RPM, as required by CMS. Store records for at least 7 years to comply with audit protocols.
- Align with chronic care: Target patients with conditions like diabetes or heart failure, where RPM demonstrably improves outcomes. Medicare prioritizes chronic care management, mirroring how industrial systems prioritize high-risk parameters (e.g., ammonia levels in wastewater).
- Train staff on billing: Assign a dedicated team member to track data transmission days and monitor time, avoiding the common pitfall of under-documenting interactive communication (a requirement for CPT 99457/99458).
Medicare’s RPM reimbursement isn’t just a payment—it’s a framework to elevate care delivery. By treating patient data with the same rigor as industrial monitoring systems, practices can turn compliance into a competitive advantage. Start small: enroll 10–20 high-need patients, validate your workflows, then scale. The 2025 Physician Fee Schedule rewards precision—measure twice, bill once.
Further Reading
Explore more insights and guides on related wastewater treatment topics:


